Landmark Ruling: Aetna Liable for Sex Discrimination Over Denial of Trans Facial Surgery


Table of Contents
ToggleYou might ask whether Aetna’s categorical refusal to cover facial feminization surgery rests on a lawful medical policy or an impermissible sex-based presumption. The judge’s order pushes you toward individualized medical-necessity determinations, not blanket exclusions framed as “cosmetic.” It ties that obligation to ACA Section 1557 and the logic of Bostock, treating gender dysphoria evidence as legally relevant. If you’ve faced a denial, the next question is what rights you can invoke and how far they reach…
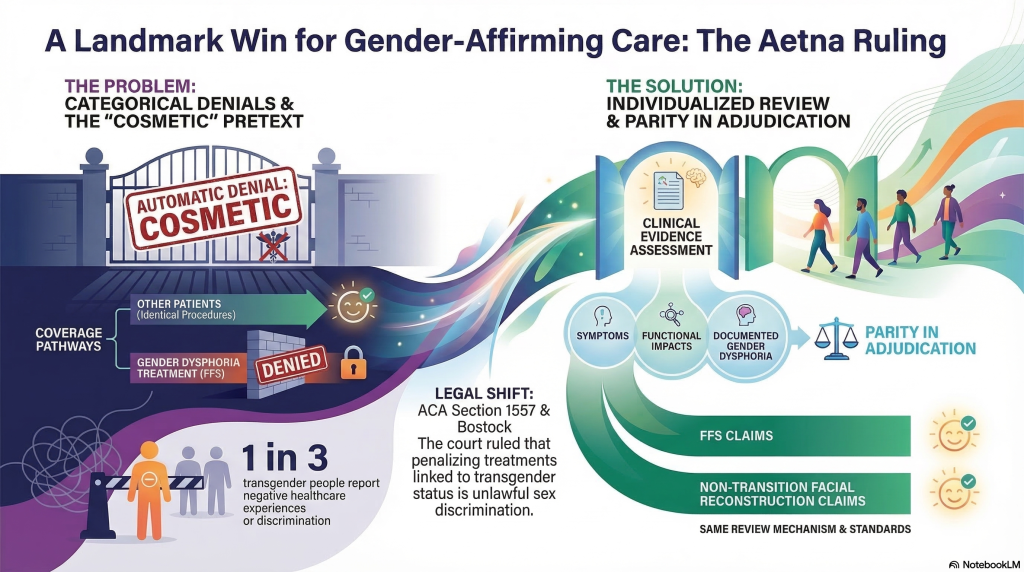

Although the injunction doesn’t force Aetna to approve facial feminization surgery across the board, it does compel the insurer to stop applying Clinical Policy Bulletin 0615 as an automatic, categorical bar and instead make individualized, medical-necessity determinations for the two plaintiffs’ facial surgery requests—treating them the way it would treat comparable facial reconstruction claims that aren’t tied to gender change. You can read the order as enforcing process rights: Aetna must consider your clinicians’ evidence, your symptoms, and functional impacts, including documented gender dysphoria, rather than presuming “cosmetic” status. You also gain parity in adjudication—Aetna must use the same standards, documentation pathways, and review mechanisms it uses for non-transition facial claims. The injunction therefore preserves access to individualized care while the case proceeds.


Because Section 1557 of the Affordable Care Act bars discrimination “on the basis of sex” in covered health programs and incorporates Title IX’s enforcement framework, it gives you a direct statutory hook to challenge an insurer’s blanket denial of facial feminization surgery as “cosmetic” when the denial turns on transgender status. You can argue the exclusion operates facially and in application as sex-based discrimination: the plan must identify you as transgender, which necessarily references sex assigned at birth, before it denies coverage. Under the Bostock precedent, penalizing you for traits or treatments linked to transgender status is sex discrimination. Section 1557 then supplies remedies and standards, so you can seek injunctive relief and individualized medical-necessity review. Those are the core ACA implications for FFS denials.
You now have stronger footing to demand an individualized, medical-necessity review for facial feminization surgery, not a categorical “cosmetic” dismissal. The court treated Aetna’s blanket exclusion as sex discrimination under ACA Section 1557, consistent with *Bostock*’s logic that unequal treatment tied to sex is unlawful. That matters: in one U.S. survey, 1 in 3 trans people reported at least one negative health-care experience. Use this precedent, document dysphoria, and appeal aggressively.
 News and AdvocacyMay 18, 2026Colorado’s Highest Court to Hospitals: Ignore Trump, Continue Gender-Affirming Care
News and AdvocacyMay 18, 2026Colorado’s Highest Court to Hospitals: Ignore Trump, Continue Gender-Affirming Care Fashion and ExpressionMay 16, 2026Shopping Made Simple: Essential Tips for Early MTF Transition
Fashion and ExpressionMay 16, 2026Shopping Made Simple: Essential Tips for Early MTF Transition Featured PostsMay 16, 2026Chasing Sanctuary: The Impact of Hostile Legislation on Transgender Migration
Featured PostsMay 16, 2026Chasing Sanctuary: The Impact of Hostile Legislation on Transgender Migration Featured PostsMay 12, 2026Trans: Learning to Be a Woman
Featured PostsMay 12, 2026Trans: Learning to Be a Woman